What is perimenopause and are you in it?
Published January 2023 | 5 min read
Expert contributor Dr Ginni Mansberg, GP
Words by Charmaine Yabsley
You’ve heard of menopause, but what about perimenopause? While every woman goes through this, not everyone knows about it. We speak to a GP for some general advice.
Menopause is the time of life when your menstrual cycle has officially stopped for a year. Perimenopause refers to the natural process leading up to menopause when your ovulation and periods may become irregular or stop.
These years can bring great change and symptoms which can affect you emotionally, mentally and physically. Some women may hardly notice any changes, but for others it can be a difficult and confusing period of life.
“Perimenopause comes at a time of your life when there’s an awful lot on,” says GP Dr Ginni Mansberg, author of The M Word. “You may be parenting teenagers; you may have parents who are getting sick; your career is probably going well and so you take on extra responsibilities – and therefore stress.”
These pressures can leave you feeling incredibly irritable, which many people put down to stress or depression. “It’s when the symptoms, especially depressive-like symptoms, become too much, that women seek advice. What most women are experiencing is not depression as many doctors may initially diagnose, but perimenopause,” says Dr Mansberg.
The biggest problem, Dr Mansberg explains, is that there is no test for perimenopause. “The data that’s emerging is that if a woman presents with perimenopausal symptoms, including depression, then they should be firstly given hormonal treatment.” In the past, she says, many women were given antidepressants, which do not address the hormonal issues women can experience during this time.

The signs and symptoms of perimenopause
The staging system devised by The University of Pennsylvania divides the menopause transition into four stages.
- Premenopause (regular menstrual cycles of 21 to 35 days).
- Early transition (there’s a decrease in predictability, and the length of a ‘usual cycle’ has changed by several days).
- Late transition (two to 11 months without a period).
- Postmenopausal (greater than or equal to 12 months of no periods).
“While menopause and perimenopause are often thrown in together, hormonally they are very different,” says Dr Mansberg. “Progesterone (a hormone involved in the menstrual cycle) steadily declines from perimenopause before your periods even start to become erratic. It finally falls close to zero as you hit menopause.”
Many studies have shown that during perimenopause your oestrogen fluctuates up and down like a yo-yo. “As your ovaries are getting a little weaker and cranking out less oestrogen, your pituitary gland in your brain leaps into gear and starts pushing out follicle-stimulating hormone (FSH). These slightly ageing ovaries will move between sluggishly ignoring the FSH, to having a massive response and pushing out stacks of oestrogen. So you can oscillate between low oestrogen and excessive oestrogen month to month, week to week, even day to day,” says Dr Mansberg.
In the final stages of perimenopause, particularly in the one to two years prior to your final period, your oestrogen levels decline and you get less episodes of the excess oestrogen, advises Dr Mansberg. “Your androgens (a sex hormone) will also have a last surge before true menopause starts.”
Around 80% of women may experience symptoms during perimenopause including:
- hot flushes
- heavy, irregular or unpredictable periods
- vaginal dryness
- insomnia
- mood problems
- exhaustion
- low libido
- loss of bone density
- weight gain
- joint pain
- incontinence
- itchy, dry skin.
Some unusual, but still experienced, symptoms, include:
- ringing in the ears or tinnitus
- heart palpitations
- dry mouth
- dry eyes
- gum and teeth problems.
There’s no specific age women begin perimenopause, as it’s different for each woman, says Dr Mansberg, “however, we know that smokers go into menopause earlier.” Around one in 12 women experience early menopause by the age of 45.
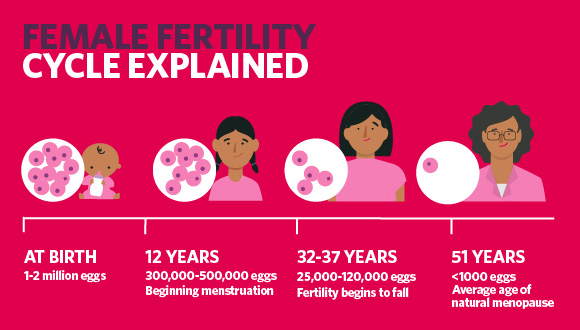
How does perimenopause impact my fertility?
If you’re in perimenopause – having irregular periods – you’re not infertile. “It’s not likely you’ll get pregnant, but it can still happen,” says Dr Mansberg. “You’re still ovulating at this time. If you’re on HRT during perimenopause, it’s important to practise safe sex if you don’t wish to fall pregnant.”
Should I see a doctor for perimenopause?
Despite the fact that women will spend one-third of their life in all of the various menopause stages, the symptoms during this time are not talked about enough. Getting help if you’re struggling has also not been encouraged enough.
“Perimenopause can easily go on for 10 years,” says Dr Mansberg. “It’s so important women get the help they need during this time.”
The most current figures show that in Australia only about 13% of menopausal women take HRT. For most women, HRT is safe and effective, adds Dr Mansberg.
There are some small risks associated with HRT, including breast cancer, blood clots, nausea, bloating, mood swings and breast tenderness. “Tweaking a woman’s dose will deal with most of these [symptoms],” says Dr Mansberg. The risk of breast cancer is small, but you should discuss your history with your GP.
What can I do at home to feel better?
“It’s important that first and foremost women get the support they need for their symptoms,” says Dr Mansberg. She agrees that while lifestyle can be a powerful tool in managing symptoms, if you’re exhausted, in pain or are lacking in motivation due to low hormones, then it can be difficult to implement these changes.
She suggests you first tackle your sleep patterns, as this will help give you the energy to do some gentle exercise or eat more healthily and avoid reaching for comfort food. “A 2mg dose – at least – of melatonin can help reset your sleep,” she says, and advises women to speak to their GP about a prescription for their needs.
To help you build better sleep habits we’ve partnered with Sleepfit Solutions, who deliver an app that can help you identify sleep issues, recommend improvements and give you access to personalised tools. Eligible members with hospital or extras cover* can get a free 12-month Sleepfit subscription.
It’s also vital to support your bone density at this time. “Weight-bearing exercises and balance-improving exercises are a must,” says Dr Mansberg. Find a gym or a trainer who understands what you need at this time of your life.
Weight gain is a symptom of perimenopause and it’s tempting to cut out food groups in an attempt to lose those unwelcome kilos. But, says Dr Mansberg, think of your bones. “Dairy and whole foods are important, especially dairy to help build bone density,” she says.
For eligible members looking for support in achieving and maintaining a healthy weight, HCF offers free access to the Healthy Weight for Life Essentials program^ to help develop healthy habits, increase energy levels, and prevent the onset of chronic conditions later on.
“Ultimately, we need to be realistic,” she says. “What works for one woman, won’t work for another. It’s more important that you are heard by your GP and you get the help and support you need.”
If you’re seeking support, talk to your partner, friends and family about your symptoms. They can help you put together a plan of action. If you’re struggling and you feel like your GP isn’t quite getting it or not hearing you, visit the Australian Menopause Society website. You can find a GP in your area who has a particular interest in perimenopause, menopause and female hormones.
Menopause Matters podcast
The journey through perimenopause and menopause can be a challenging but also a liberating time – physically, mentally and emotionally.
In our Menopause Matters podcast, join host Alison Brahe-Daddo as she unpacks the experience of this life-changing yet entirely normal part of life. Speaking with leading menopause experts, Alison sheds light on issues faced by many women, including some of the best ways to manage your symptoms, how to navigate your career, mental health and relationships during this time, and shares the joys of life post-menopause.
RELATED ARTICLES
Relieving menopause symptoms
If you’re approaching or experiencing menopause, you’re probably aware of how it can affect your mind and body. Here’s how to manage the symptoms.
How to deal with depression
Don’t deal with depression alone. There are many ways to lessen symptoms to live a happier, healthier life.
Tackle your sleep problems
There are plenty of simple sleep strategies to help you get more restorative shut-eye – all night long.
Why am I always tired?
Finding it hard to keep your eyes open? We explore six of the most common causes of tiredness and what you could do about them.
Important Information
* Eligibility criteria apply. See hcf.com.au/sleepfit for details.
^ Eligibility criteria applies. For more information see hcf.com.au/hwfl
This communication contains information which is copyright to The Hospitals Contribution Fund of Australia Limited (HCF). It should not be copied, disclosed or distributed without the authority of HCF. Except as required by law, HCF does not represent, warrant and/or guarantee that this communication is free from errors, virus, interception or interference. All reasonable efforts have been taken to ensure the accuracy of material contained on this website. It’s not intended that this website be comprehensive or render advice. HCF members should rely on authoritative advice they seek from qualified practitioners in the health and medical fields as the information provided on this website is general information only and may not be suitable to individual circumstances or health needs. Please check with your health professional before making any dietary, medical or other health decisions as a result of reading this website.