What is chemotherapy?
Chemotherapy is a common cancer treatment: we explain what it involves and the different forms it can take.
Dr Lindy Alexander
March 2018
It’s a sad fact that 1 in 2 Australian men and women will be diagnosed with cancer if they live to the age of 85. And while not everyone who’s diagnosed with cancer will be given chemotherapy, “In 2014-15 chemotherapy was the most common cancer treatment recorded as the principal reason for hospitalisation,” says CEO of Cancer Council Australia, Professor Sanchia Aranda.
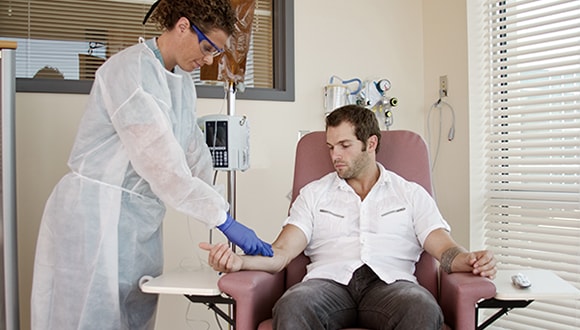
What is chemotherapy?
Chemotherapy is the use of anti-cancer drugs to kill or slow the growth of cancer cells. The drugs used during chemotherapy enter the bloodstream and travel throughout the body to reach and destroy cancer cells in organs and tissues to stop them reproducing.
Chemotherapy is a category of more than 100 different drugs. Your oncologist (a doctor who specialises in the diagnosis and treatment of cancer) will choose which drug(s) to give based on the type and stage of your cancer.
What does chemotherapy do?
“Chemotherapy can be used to treat the cancer or to ease the symptoms of cancer,” says Prof Aranda.
According to Cancer Council Australia, chemotherapy can be used to:
- achieve remission (when the signs and symptoms of cancer reduce or disappear). This is called curative chemotherapy and may be used with other treatments, such as surgery and radiotherapy.
- help other treatments. In this case it may be used before or after another treatment.
- stop the cancer spreading and relieve symptoms – this may be called palliative chemotherapy.
- stop the cancer coming back – this is called maintenance chemotherapy and may be given for months or years after you’re in remission. It aims to prevent or delay the cancer returning.
What’s involved with chemotherapy treatment?
Your doctor will discuss your treatment plan with you, as it’s not the same for everyone. Most people have chemotherapy during day visits to a hospital or a treatment centre. According to Prof Aranda, your stay may range from a few minutes to several hours.
Treatment sessions to destroy all the cancer cells may be daily, weekly or monthly and may last anywhere from 3 months to a year. “How often and for how long a person has chemotherapy depends on the type of cancer you have and the drugs that are used,” says Prof Aranda.
Chemotherapy may be given orally; through an intravenous device placed in a large vein, usually in the neck or chest which may remain there throughout the course of the treatment; by injecting drugs directly into an organ or tissue affected by cancer; or as a cream, reports Cancer Council Australia.
What are the side effects of chemotherapy?
Because there are many different forms of chemotherapy, different people may have different treatment and therefore different side effects.
Chemotherapy drugs damage cells as they divide (cancer cells divide more rapidly than most normal cells). However some other cells – such as hair follicles, blood cells and cells inside the mouth and bowel – also divide rapidly so can be affected by chemotherapy. Side effects occur when chemotherapy damages these normal cells, but as they can recover, the side effects are temporary.
Common side effects include:
- Hair loss – not all chemotherapy drugs cause hair loss, but many can. “Sometimes all the hair is lost, or sometimes it just gets thinner,” says Prof Aranda. “Hair can be lost from all parts of the body with chemotherapy.”
- Weight loss – chemotherapy won’t necessarily make a patient lose weight. Some drugs, like hormone therapy and medicines, such as steroids, can actually increase your appetite or cause the body to retain fluids, causing weight gain. Though for others, the type of cancer and its treatment can make it hard for patients to eat well and take in the nutrients required to maintain weight.
- Nausea and vomiting – while these are unpleasant and uncomfortable side effects, there are anti-nausea treatments available to help and provide relief.
- Fatigue – Prof Aranda says “It’s important that people undergoing chemotherapy have a good balance of activity and rest, and plan for some modification of their usual routines to ensure they can maintain wellbeing.”
- ‘Chemo-brain’ – Chemo brain is described as feelings of not remembering things, feeling vague or having trouble concentrating. Research has not been able to determine the causes of chemo brain.
Can you still work when having treatment?
“Whether you can work during treatment will depend on the type and stage of cancer, the type of treatment you have and its side effects, how you feel during treatment and the kind of work you do,” says Prof Aranda.
“Each person’s situation is different – not everyone with the same type of cancer will make the same decision about work.” Talk to your oncologist or treatment team about what’s right for you.
What are the costs involved?
The Australian Government may help cover some of your chemotherapy costs if you have a current Medicare card. Ask your hospital or treatment centre about the fees.
Certain private health packages can also help to cover some cancer treatments, depending on your level of cover. Call us on 13 13 34 to find out more.
Where can I go for support?
Cancer Australia has a list of cancer support organisations, including your local Cancer Council resources and other foundations.
You can also call Cancer Council on 13 11 20 Monday – Friday.
Related articles
PERSONALISING BREAST CANCER TREATMENT FOR BETTER RESULTS
Future breast cancer treatments are evolving towards targeted therapies individualised for each patient’s condition.
TACKLING OUR HEALTH CRISIS
The Australian Partnership Prevention Centre is working on solutions to halt the increasing trend of chronic health conditions.
HEALTH CHECKS BY AGE: THE TESTS YOU SHOULD BE HAVING
Your guide to staying on top of your health, through every stage of life.
SERIOUS CONDITIONS THAT CAN BE MISSED
Many serious conditions have vague or hidden symptoms. Here’s how to identify and screen for them.